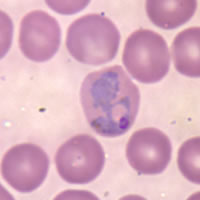
Malaria
|
|
Malaria (Italian: "bad air"; formerly called ague or marsh fever in English) is an infectious disease which in humans causes about 350-500 million infections and over 1 million deaths annually, mainly in the tropics and sub-Saharan Africa.
Malaria is caused by the protozoan parasite, Plasmodium (one of the Apicomplexa) and the transmission vector for human malarial parasite is the Anopheles mosquito. The P. falciparum variety of the parasite accounts for 80% of cases and 90% of deaths.
For his discovery of the cause of malaria, French army doctor Charles Louis Alphonse Laveran was awarded the Nobel Prize for Physiology or Medicine in 1907.
Symptoms of malaria include fever, shivering, arthralgia (joint pain), vomiting, anemia, and convulsions. There may be the feeling of tingling in the skin, particularly with malaria caused by P. falciparum. Complications of malaria include coma and death if untreated—young children are especially vulnerable.
| Contents |
Mechanism of the disease
Infected female Anopheles mosquitoes carry Plasmodium sporozoites in their salivary glands. If they bite a person, which they usually do starting at dusk and during the night, the sporozoites enter the person's body via the mosquito's saliva, migrate to the liver where they multiply within hepatic liver cells. They then turn into merozoites which then enter red blood cells. There they multiply further, periodically breaking out of the red blood cells. The classical description of waves of fever coming every three or four days arises from simultaneous waves of merozoites breaking out of red blood cells during the same day.
The parasite is relatively protected from attack by the body's immune system because it stays inside liver and blood cells. However, circulating infected blood cells are killed in the spleen. To avoid this fate, the parasite produces certain surface proteins which infected blood cells express on their cell surface, causing the blood cells to stick to the walls of blood vessels. These surface proteins known as PfEMP1 are highly variable (there are at least 50 variations) and cannot serve as a reliable target for the immune system.
By the time the human immune system learns to recognise the protein and starts making antibodies against it, the parasite has switched to another form of the protein, making it difficult for the immune system to keep up.
The stickiness of the red blood cells is particularly pronounced in Plasmodium falciparum malaria and this is the main factor giving rise to hemorrhagic complications of malaria.
Some merozoites turn into male and female gametocytes. If a mosquito bites the infected person and picks up gametocytes with the blood, fertilization occurs in the mosquito's gut, new sporozoites develop and travel to the mosquito's salivary gland, completing the cycle.
Pregnant women are especially attractive to the mosquitoes, and malaria in pregnant women is an important cause of stillbirths and infant mortality.
The recognised species causing disease in humans are P. falciparum (which alone accounts for 80% of the recognised cases and ~90% of the deaths) and P. vivax, but P. ovale, P. malariae, P. knowesli and P. semiovale are also known to cause malaria.
High endothelial venules can be occluded by the infected red blood cells, such as in placental and cerebral malaria. In cerebral malaria the sequestrated red blood cells affect the integrity of the blood brain barrier possibly leading to reversible coma. Even when treated, serious neurological consequences may result from cerebral malaria, especially in children.
Other mammals (bats, rodents, non-human primates) as well as birds and reptiles also suffer from malaria. However, the form of malaria found in animals is usually different than that found in humans. Three human forms (which account for most malaria cases) are completely exclusive to humans. Only one form, P. malariae, can cause malaria in both humans and higher primates. Other animal forms of malaria do not infect humans at all. Mosquitos which are "virgin" (i.e. have never bitten someone before) cannot transmit malaria, even if the eggs were laid by a female carrier of the disease.
Sickle cell anemia and other genetic effects
Carriers of the sickle cell anemia gene are protected against malaria because of their particular hemoglobin mutation; this explains why sickle cell anemia is particularly common among people of African origin. There is a theory that another hemoglobin mutation, which causes the genetic disease thalassemia, may also give its carriers an enhanced immunity to malaria.
Another disease that gives protection against malaria is glucose-6-phosphate dehydrogenase deficiency (G6PD). It protects against malaria caused by Plasmodium falciparum as the presence of this enzyme is critical to survival of these parasites within red blood cells.
It is thought that humans have been affected by malaria for about 50,000 years, and several human genes responsible for blood cell proteins and the immune system have been shaped by the struggle against the parasite.
Treatment and prevention
If diagnosed early, malaria can be treated, but prevention is always much better, and substances that inhibit the parasite are widely used by visitors to the tropics. Since the 17th century quinine has been the prophylactic of choice for malaria. The development of quinacrine, chloroquine, and primaquine in the 20th century reduced the reliance on quinine. These anti-malarial medications can be taken preventively, which is recommended for travellers to affected regions.
Certain strains of Plasmodium have recently developed resistance to chloroquine, which was the first line of treatment in many countries, thus complicating the treatment. In West Africa, where the local strains of malaria are particularly virulent, mefloquine (trade name Lariam) is now the recommended prophylactic, despite causing psychological problems in some vulnerable people. Doxycycline, an antibiotic, is also prescribed as a prophylactic against quinine-resistant malaria, though its use is less common than Lariam because it must be consumed daily. It seems inevitable that resistance to these drugs will also occur. "Malarone" is also a recommended prophylactic.
Extracts from the plant Artemisia (specifically Artemisia annua), containing the compound artemisinin, a substance unrelated to the quinine derivatives, offer over 90% efficacy rates but their supply is not meeting demand. On June 5, 2005 Nature (journal) released a study about possible drug resistance, although the finding could help the development of other drugs. [1] (http://news.bbc.co.uk/1/hi/health/4615023.stm)
In addition to the antimalarial drugs, the use of mosquito repellents such as DEET, and mosquito nets and screens can reduce the chances of contracting malaria, as well as the discomfort of insect bites.
Disease control
Background
Efforts to eradicate malaria by eliminating mosquitos have been successful in some areas. Malaria was once common in the United States and southern Europe, but the draining of wetland breeding grounds and better sanitation eliminated it from affluent regions. Malaria was eliminated from the northern parts of the USA in the early twentieth century, and the use of the pesticide DDT during the 1950s eliminated it from the South. A major public health effort to eradicate malaria worldwide by selectively targeting mosquitos in areas where malaria was rampant was embarked upon in the 1950s and 1960s. (The Mosquito Killer (http://www.gladwell.com/2001/2001_07_02_a_ddt.htm)—PDF of the same article (http://www.gladwell.com/pdf/malaria.pdf)) However, these efforts ultimately failed to eradicate malaria in many parts of the developing world.
DDT was developed as the first of the modern insecticides early in World War II. It was initially used with great effect to combat mosquitoes spreading malaria. It was banned for use in many countries in the 1970s due to its negative environmental impact. There is great controversy regarding this impact and the use of DDT to fight human diseases. Some claim that the ban is responsible for malaria deaths counted in tens of millions in tropical countries where the disease had been under control.
The World Bank estimates that malaria costs Africa $12bn a year in lost productivity. Yet international funding for malaria control is only $100m-$200m a year.[2] (http://www.guardian.co.uk/international/story/0,,1502272,00.html) It has been argued that in order to meet the Millennium Development Goals, money should be redirected from HIV/AIDS treatment to malaria prevention, which for the same amount of money would provide much greater benefit to African economies.
Conventional means
Since most of the deaths today occur in poor rural areas of Africa which lack health care, the distribution of mosquito nets impregnated with insect repellants has been suggested as the most cost-effective prevention method. These nets can often be obtained for less than US$10 or 10 euros when purchased in bulk from the United Nations or other organizations. The nets need to be re-impregnated with the chemical about every six months.
Spraying interior walls with DDT is also effective in areas where the mosquitoes are not already DDT-resistant. This public health use of small amounts of DDT is permitted under the Stockholm Convention on persistent organic pollutants (POPs), which prohibits the agricultural use of DDT [3] (http://www.pops.int/) for large-scale field spraying.
Vaccines and other new techniques
Vaccines for malaria are under development, with no completely effective vaccine yet available (as of November 2004). A team backed by the Gates Foundation and the pharma giant GlaxoSmithKline announced a partially successful field trial in October 2004, for RTS,S/AS02A, a vaccine which reduces infection risk by 30% and severity of infections by over 50% [4] (http://www.malariavaccine.org). Further research will delay this vaccine from commercial release until around 2010. In January 2005, Edinburgh University scientists announced the discovery of an antibody which protects against the disease. The scientists will lead a £17m European consortium of malaria researchers [5] (http://news.scotsman.com/scotland.cfm?id=56062005). It is hoped that the genome sequence of the most deadly agent of malaria, Plasmodium falciparum, which was completed in 2002, will provide targets for new drugs or vaccines.
Sterile insect technique is emerging as a potential method to control malaria-carrying mosquitos. Progress towards transgenic, or genetically modified insects suggests that wild mosquito populations could be made malaria-resistant. Researchers at Imperial College London created the world's first transgenic malaria mosquito [6] (http://www.ic.ac.uk/templates/text_3.asp?P=1911), with the first plasmodium-resistant species announced by a team at Case Western Reserve University in Ohio in 2002 (See Jacobs-Lorena et al, 2002) [7] (http://www.cwru.edu/pubaff/univcomm/2002/may/mosquito.htm).
A very promising approach was announced in Science on June 10 2005. It uses inert spores of the fungus Beauveria bassiana to kill mosquitoes, sprayed on walls and bed nets. Unlike chemicals, mosquitoes have never been found to develop a resistance to fungal infections. BBC report (http://news.bbc.co.uk/1/hi/health/4074212.stm) Times report (http://www.timesonline.co.uk/article/0,,2-1647983,00.html)
Travel to malaria-risk zones
Travelers to malaria-risk zones should first contact a physician whose speciality is in travel medicine. Most often a general practitioner cannot prescribe medications or give vaccinations for third-world travel. Seldom will malaria be the sole health concern, and the physician will need to assess all the health risks the traveler will face. There are several drugs available for malaria prevention (many are also used in higher doses for treatment) including quinine, mefloquine, doxycycline, and Malarone. There is no one drug that is right for all travelers to all destinations. The choice of a malaria prophylaxis should be made carefully with one's physician taking into account drug resistance in the traveler's destination; possible side effects, interactions, and contraindications; and finally the preferred frequency per dose (daily, weekly, etc.). Non-generic drugs such as Malarone tend to be quite expensive, so time permitting, the traveler may wish to compare prices at various pharmacies.
Travel to rural areas always involves more potential exposure to malaria that in the larger cities. (This is in contrast to dengue fever where cities present the greater risk.) For example, the capital cities of the Philippines, Thailand and Sri Lanka are essentially malaria-free. However, malaria is present in many other places (especially rural areas) of these countries. By contrast, in West Africa, Ghana and Nigeria have malaria throughout the entire country. However, the risk will always be lower in the larger cities. Travelers should never assume that their choice of malaria prophylaxis is available in the country that they will be visiting. In most third-world countries only quinine (and possibly doxycycline) are available, even though the malaria there may be resistant.
Any malaria prophylaxis must be taken before, during, and (especially) after traveling to a malaria-risk zone. The exact frequency will vary by which drug is chosen. There has been some debate recently over whether pre-travel malaria prophylaxis is being started early enough. For example, mefloquine is normally taken one week prior to travel. Some feel this is inadequate if the person is unfortunate enough to be exposed to malaria shortly upon arrival. Those who have concerns may wish to discuss with their physician about doubling the time period (not the dosage) that their malaria prophylaxis will be taken prior to travel. In addition to providing better protection, there will be more time to switch to another anti-malaria medication, if necessary.
No malaria prophylaxis is 100% effective in prevention. Avoiding mosquito bites (i.e. using DEET, screens, and proper bed netting) when mosquitos are obviously present is important as well. If a person who has visited a malaria risk zone contract a fever within one year, their physician should be informed of the possibility of malaria. Note that lesser forms of malaria (such as P. vivax) can mimic the symptoms of the flu. Physicians who rarely, if ever, examine malaria patients may need to be reminded of this fact. The standard laboratory test for malaria is a thick and thin blood smear on a glass slide viewed under the microscope.
Aspirin must never be taken as an antipyretic when malaria or dengue fever is a possibility. (Continuing daily low-dose 81 mg aspirin therapy during and after third-world travel should be discussed with your physician.) Acetaminophen and ibuprofen are considered safe alternatives provided all of their precautions are observed. Malaria, dengue fever, and typhoid fever all tend to have somewhat similar symptoms at first and should not be self-diagnosed.
References
- Ito J, Ghosh A, Moreira LA, Wimmer EA, Jacobs-Lorena M. Transgenic anopheline mosquitoes impaired in transmission of a malaria parasite. Nature 2002;417:387-8. PMID 12024215
External links
- WHO site on malaria (http://mosquito.who.int/malariacontrol)
- CDC site on malaria (http://www.cdc.gov/malaria/)
- Medline Plus site on malaria (http://www.nlm.nih.gov/medlineplus/malaria.html)
- LookSmart - Malaria (http://search.looksmart.com/p/browse/us1/us317837/us317920/us53948/us931698/us948221/us927213/us948384/us274409/) directory category
- Open Directory Project - Malaria (http://dmoz.org/Health/Conditions_and_Diseases/Infectious_Diseases/Parasitic/Malaria/) directory category
- Yahoo! - Malaria (http://dir.yahoo.com/Health/Diseases_and_Conditions/Malaria/) directory category
Vaccine and other research
- Malaria Vaccine Initiative (http://www.malariavaccine.org)
- Wellcome Trust against Malaria (http://www.wellcome.ac.uk/en/malaria/)
- New Scientist - New Malaria Vaccine Raises High Hopes (http://www.newscientist.com/news/news.jsp?id=ns99996537) 15 October 2004
- BBC - Hopes of Malaria Vaccine by 2010 (http://news.bbc.co.uk/2/hi/health/3742876.stm) 15 October 2004
- Malaria. The UNICEF-UNDP-World Bank-WHO Special Programme for Research and Training in Tropical Diseases (http://www.who.int/tdr/diseases/malaria/default.htm)
- story of the discovery of the vector of the malarial parasite (http://stevenlehrer.com/explorers/chapter_6-5.htm)
- History of discoveries in malaria (http://www.malariasite.com/malaria/History.htm)
- History of Malaria in Spain (http://www.iberianature.com/material/malaria.html)
- BBC - Science shows how malaria hides (http://news.bbc.co.uk/1/hi/health/4419835.stm) 8 April 2005
DDT
- The DDT Ban Myth (http://info-pollution.com/ddtban.htm)
Animations, images and photos
- Burden of Malaria (http://news.bbc.co.uk/2/shared/spl/hi/picture_gallery/05/world_burden_of_malaria/html/1.stm), BBC pictures relating to malaria in northern Uganda
- Malaria: Cooperation among Parasite, Vector, and Host (Animation) (http://www.sumanasinc.com/scienceinfocus/sif_malaria.html)ca:Malària
da:Malaria de:Malaria es:Malaria fr:Paludisme he:מלריה ia:Malaria ms:Malaria nl:Malaria ja:マラリア no:Malaria pl:Malaria pt:Malária sl:Malarija su:malaria sv:Malaria zh:疟疾